Common Infectious Diseases
- Actinomyces
- (Coccobacillus) Bacterial Vaginosis
- Candidiasis
- Gardnerella
- Herpes Simplex Virus
- Trichomoniasis
Actinomyces
 Actinomyces is a gram-positive, anaerobic, rod bacteria. The most common predisposing factor is the duration of IUD use. The type of IUD does not influence the presence of this bacteria.
Actinomyces is a gram-positive, anaerobic, rod bacteria. The most common predisposing factor is the duration of IUD use. The type of IUD does not influence the presence of this bacteria.
Most women who are positive for actinomyces infection are asymptomatic. Although this bacteria is generally commensal, there are reported cases of actinomyces causing pelvic inflammatory disease (PID) in women who have IUDs.
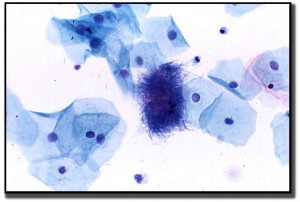
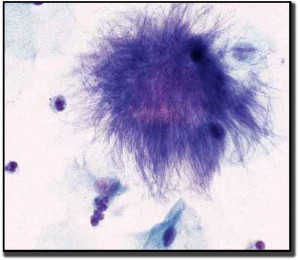 Actinomyces look like a cotton ball, or a woolly, fuzzy mass. The organisms are tangled clumps of rods of varying lengths and exhibit acute angle branching, non-spore-forming bacilli.
Actinomyces look like a cotton ball, or a woolly, fuzzy mass. The organisms are tangled clumps of rods of varying lengths and exhibit acute angle branching, non-spore-forming bacilli.
An acute inflammatory response is usually present.
Clinical signs and symptoms:
-
Lesions on the cervix appear yellow and granular to the naked eye.
-
Chronic infection of the cervix may produce significant fibrosis and scarring.
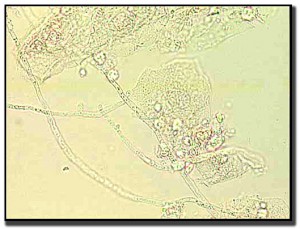
Candidiasis spp.
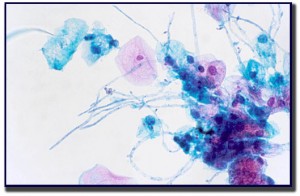 Candida albicans is responsible for 80-92% of the candida infections. Candida, or fungus, is present as part of the normal vaginal flora in 15-20% of healthy women and in up to 30-40% of pregnant women. Factors that predispose women to candida are: pregnancy, diabetes, HIV infection, oral contraceptives, antibiotic or corticosteroid use, immunosuppression, and history of recurrent candida.
Candida albicans is responsible for 80-92% of the candida infections. Candida, or fungus, is present as part of the normal vaginal flora in 15-20% of healthy women and in up to 30-40% of pregnant women. Factors that predispose women to candida are: pregnancy, diabetes, HIV infection, oral contraceptives, antibiotic or corticosteroid use, immunosuppression, and history of recurrent candida.
Other factors that may increase the incidence of candida include the use of douches, perfumed feminine hygiene sprays, topical antimicrobial agents, and tight, poorly ventilated clothing and underwear.
Microscopic examinations of saline and KOH preparations will reveal budding yeast cells in approximately 50-70% of yeast infections.
A wet smear is made from the exudate, and 10-20% KOH is added to the preparation. The fungi will appear in the form of long, thread-like fibers and may have attached tiny buds. Lactobacillus is almost always absent in a smear with candida present.
Clinical signs and symptoms:
- Non-malodorous, thick, white, cottage cheese-like discharge
- Vaginitis
- Pruitus in vulvar area together with erythema of vagina or vulva
- Identifying candida in the absence of symptoms should not lead to treatment
- pH less than 4.5
- Moist atmospheres
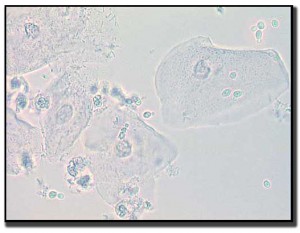
Coccobaccillus (bacterial vaginosis)
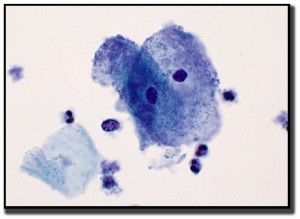 Bacterial vaginosis is not a sexually transmitted infection (STI), but it is linked to sexual activity. Bacterial vaginosis is the most common vaginal condition in women of reproductive age and is treated with antibiotics like Clindamycin. On cytology reports, this finding is stated as “a shift in vaginal flora consistent with coccobaccilli spp.”
Bacterial vaginosis is not a sexually transmitted infection (STI), but it is linked to sexual activity. Bacterial vaginosis is the most common vaginal condition in women of reproductive age and is treated with antibiotics like Clindamycin. On cytology reports, this finding is stated as “a shift in vaginal flora consistent with coccobaccilli spp.”
On cytology we observe an absence of lactobacilli; however, small coccobacilli are evident. Squamous cells that are covered by a layer of coccobacilli—especially along the margin of the cell membrane, uniformly spaced, and grainy-appearing—are referred to as “clue cells.” There are also clumps of small rods seen in the background.
Clinical signs and symptoms:
Clinical criteria require three of four signs/symptoms
- Homogeneous, white/gray non-inflammatory discharge that adheres to vaginal walls
- Presence of clue cells on wet mount
- Vaginal pH greater than 4.5
- A fishy odor before or after addition of KOH/whiff test (KOH = potassium hydroxide)
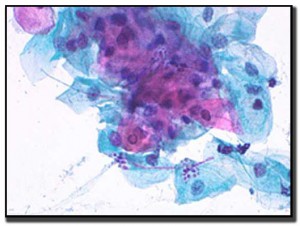
Herpes Simplex Virus
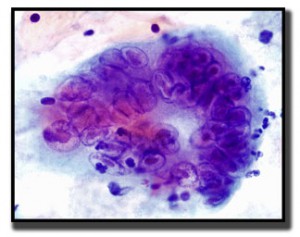 Herpes simplex virus (HSV) can maintain a latent state for the lifetime of the host.
Herpes simplex virus (HSV) can maintain a latent state for the lifetime of the host.
Virus-infected cells are usually found at the edge of and in the base of lesions. When herpes manifests on the mucosa of the labia, vagina, or both, the infection presents as vesicles. Cervical and vulva involvement is not uncommon.
Both HSV1 and HSV2 have the same cytologic impression.
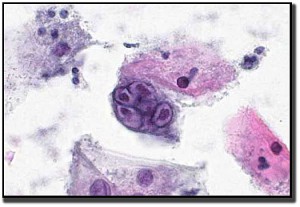
The virus causes problems with mitosis in that the nucleus replicates, but the cell doesn’t divide properly. This leads to multinucleated cells. The chromatin of the nucleus marginates to the nuclear membrane. The nuclei also tend to mold around each other in order to fit within the cell membrane.
Clinical signs and symptoms:
Most infections with herpes simplex are asymptomatic. The host immune response appears to play a major role. The incubation period is 2-11 days (usually 6-7 days). Infected individuals are most infectious during the early days of a primary infection, although the virus may still be transmitted late in the infection, or from an asymptomatic person.
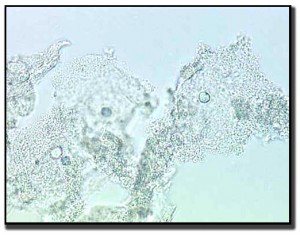
Trichomoniasis
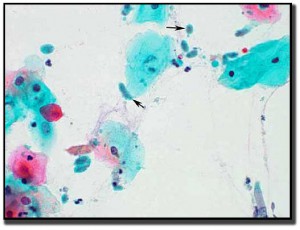 Trichomoniasis is transmitted by sexual contact. Treatment is incomplete unless all partners are also treated. Trichomoniasis is a protozoan. It is estimated that one in five people will be infected with trichomoniasis in their lifetime. Trichomoniasis is transmitted generally by physical contact and does not survive long outside the host.
Trichomoniasis is transmitted by sexual contact. Treatment is incomplete unless all partners are also treated. Trichomoniasis is a protozoan. It is estimated that one in five people will be infected with trichomoniasis in their lifetime. Trichomoniasis is transmitted generally by physical contact and does not survive long outside the host.
Clinical signs and symptoms:
- Often vaginal discharge is foul in odor, copious, frothy and yellow-gray or green in color
- Vulovaginal irritation and pruritus
- Pain on intercourse
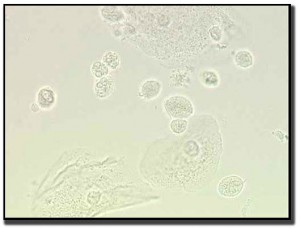
Like candida and coccobaccillus infections, trichamonas can also be seen using a wet prep. The cells are oval to round with a pear-shaped nucleus. On wet preps, the protozoan movement by the flagella is easily identified.